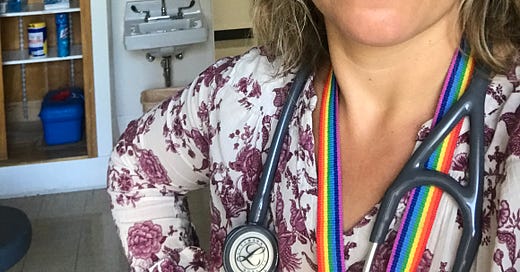
"It’s very affirming. I know that I’m exactly where I need to be."
A nurse at a clinic in Colorado doubles down on her commitment to serving the most vulnerable.
Hi folks,
I’m Rachel Halliday, the other half of “The Other Side of This”.
When Erin and I aren’t working together, I’m a political science student at Tufts and a coxswain on the men’s rowing team.
I’ve been home since March living with my twin sister and my parents. We’re close-knit, so being together all.the.time. has actually been pretty fun, but I miss my extended family members. All 46 of them.
Today, we’re interviewing my favorite cousin-in-law, Meg Champion. Meg has been an ER nurse, a Nurse Practitioner for the Denver Broncos, and is now a clinical director at a federally-funded, nurse-run clinic in Littleton, CO.
She understands the inequities in our healthcare system, cares for her patients with immense compassion, and knows how to advocate for those she serves.
We need more Megs in this world.
- Rachel
Name: Megan Champion
Hometown: Madison, Connecticut
Current Residence: Littleton, Colorado
Living Situation: House with husband and two young children
Age: 36
Occupation: Nurse Practitioner and Clinical Director, Sheridan Health Clinic at University of Colorado; I’m a bilingual healthcare provider working closely with Latinx immigrants. I specialize in women’s health.

Photo caption: This is me in the clinic.
Tell us about the clinic you work at and the types of patients you serve.
I’m a Family Nurse Practitioner, but before that I was a bedside nurse for eight years in ICU and emergency. Now I’m the clinical director of a small, federally-qualified health center, so we get money from the government to take care of folks on Medicaid or people without insurance. We are affiliated with the University of Colorado College of Nursing, and we are nurse-run; we only have one physician on staff two hours per week to sign paperwork that we’re not legally allowed to sign.
The other unique thing about our clinic is that we have an Integrated Care model. We’re a medical home: we have four Family Nurse Practitioners, two Pediatric Nurse Practitioners, two Psychiatric Nurse Practitioners and seven Behavioral Health Providers. We provide dental care, obstetric and prenatal care, substance abuse treatment, mental health treatment, pediatrics, and we have an on-site pharmacy. So, we have this integrated model where if you come to our clinic we try and support the entire person.
Demographic-wise, less than 10% of our patients have commercial insurance, our largest payer is Medicaid. We also have very few patients over the age of 65 compared to other clinics. 65% of our patients identify as Latinx or Hispanic, and more than 50% are best served in a language other than English. Around 10% of our patients are experiencing homelessness, and most of those are our teenagers, so we have a specific program for our homeless teenagers, and we have a school-based health clinic.
How has your patient population been impacted by COVID?
Where to begin...I feel like it’s so different from the white person’s experience with COVID, so I want to represent it responsibly.
The salient thing was that so many of our undocumented patients were afraid to come to the clinic; it became a ghost town. We initially assumed it was people just being responsible and staying home, but truthfully it was a response to curfew, to an increased police presence, the fact that people could be stopped without reason. There was definitely an increased ICE presence, and they threatened to come anywhere, even into healthcare clinics, to apprehend folks. So that was significant in the fact that we had trouble even getting people to respond to phone calls, knowing that they were due to come in for their diabetes medication or other care. Engaging the Latinx population in telehealth was a challenge because people were fearful of being recorded and having an image of their face or their family that they feared could be used against them.
We also do a lot of substance use disorder treatment, and so seeing domestic violence and substance use disorder increase was a reality for sure. It’s important to note, though, that our substance use population and our Latinx population are distinct groups: my Latinx patients, whether they’re documented or undocumented, are hardworking people that just want to take care of their hypertension. They come to their appointments. They return your calls. They just want their healthcare.
I feel like a lot of people think that politics doesn’t really intersect with healthcare work, but in reality your work is highly political. Can you talk about that?
It cannot be overstated how damaging the Trump administration has been to the Latinx population, the transgender population, just horrifyingly and directly damaging to everyone I serve.
I understand the implications of Medicaid and reimbursement, and I engage in political discussions about legislation that affect our patients’ access to care. I’m part of a community health network in Colorado where we’re side by side with all the other federally qualified clinics in the area, trying to figure out how to serve our population and our demographic during these times, and legislation and politics are a huge part of that.

Photo caption: My amazing quarantine garden.
If you could wave a magic wand, what would you change about healthcare policy today?
I truly think that integrated healthcare clinics like ours are able to effectively reach and serve the population, there just aren’t enough of them.
We’ve got sliding scale discount fees for people that don’t have insurance. A social security number is not required. Having folks on staff that look like you and speak your language provide these services, and that’s critical. This integrated care model is so important; it’s essential to have behavioral health services co-located with health care.
How has the pandemic affected how you see your chosen career path?
It’s very affirming. I know that I’m exactly where I need to be.
Your first healthcare job out of grad school was serving the Denver Broncos. Serving elite athletes is the polar opposite of what you’re doing now. Can you talk about your reflections on that experience?
It’s really hard to talk about.
Their cafeteria is better than many of our school systems. The elitism is profound, deeply entrenched, and my view of the NFL has changed over the course of the last three years.
When you are looking at the politics of these settings, the things that you learn over time about how certain NFL teams support Trump monetarily versus folks like Colin Kaepernick, who isn’t even able to express his political freedom within the system, you start to see the balance of power a little bit better than when you look from a bird’s eye view at an industry that primarily makes its money off of Black athletes.
On top of that, the health problems were so vastly different.
There was such serious entitlement and an entirely different view to healthcare; our clinic was located in a suburb of Denver that served an affluent, largely white community [in addition to providing primary care to the Broncos]. This population was well-educated and resource-rich, but they were difficult to serve. They often tried to dictate to me what care they should receive, and they weren’t open to education about how they could alter their lifestyle habits.
What kind of permanent changes do you see for the medical industry and best practices for care?
I think that psychiatric care and behavioral health will continue to operate over telehealth, it’s just another way we can reduce barriers to care, and it’s more comfortable for a lot of people to be in their own home and not have to travel. But for the medical industry in general this launch into virtual medicine was a blessing. A lot of clinics like mine weren’t sure how to tackle the details, but when we were forced to do so, we saw that virtual care is a great tool.

Photo caption: These are the COVID Response RN’s at our clinic.
What do you want to take to the other side of this?
I feel like the further away you are from privilege, the more able you are to realize that other people have it worse than you. It’s a shocking phenomenon that the more we have, the less willing we are to part with. We become uncomfortable so quickly, even with just a small degree of inconvenience. So, reflecting on my white privilege, no matter how bad it feels or the personal struggles I’m dealing with that day, is probably what I most want to take to the other side. It’s easy to say you don’t have it that bad, but really internalizing that gratitude and the reality of the political climate we’re seeing unfold is so important for me.
Professionally, I want to take my understanding of how impactful our clinic can be. I have a new appreciation for the force in the community we can be if we are thoughtful and responsive. It’s a cool, empowering, humbling experience to play this role for this population.